This is the second entry in a four-part series on my perianal disease timeline, including the healing after my proctectomy. Part 1 can be found HERE.
Surgery and the First month (Nov 7, 2013 – early December 2013)I’ve already written about my hospital experience following my proctectomy, so if you’re interested in reading it, please check it out HERE.
The following will detail my experiences in the first month after surgery.
My surgery was performed on the morning of Nov 7, 2013. It was the complete removal of my rectum and anus. Since I have Crohn’s disease, there would be no chance of being able to hook my small intestine up to my rectum in the future, which is often an option for people with Ulcerative Colitis.
Considering the severe damage to that area, these parts of me had no chance of ever being healthy. I was opened up again through the abdomen for this surgery. I don’t know if it can be done completely laparoscopically or not, but if my rectum was as inflamed as my colon was, then it needed more space to be pulled out.
I was discharged on Nov 12, 2013 and had a nurse come to my home in order to pack my wound until I received a wound VAC at home.
The daily wound packing was quite uncomfortable, and my nurse said that my wound would bleed easily when she removed the dressing.
I was still on morphine tablets and Tylenol, but they did little to help with the wound packing pains.
Packing the wound generally took about 15 minutes.
The old packing would be removed, the wound would be flushed with sterile water or saline, then a new ribbon packing would be inserted.
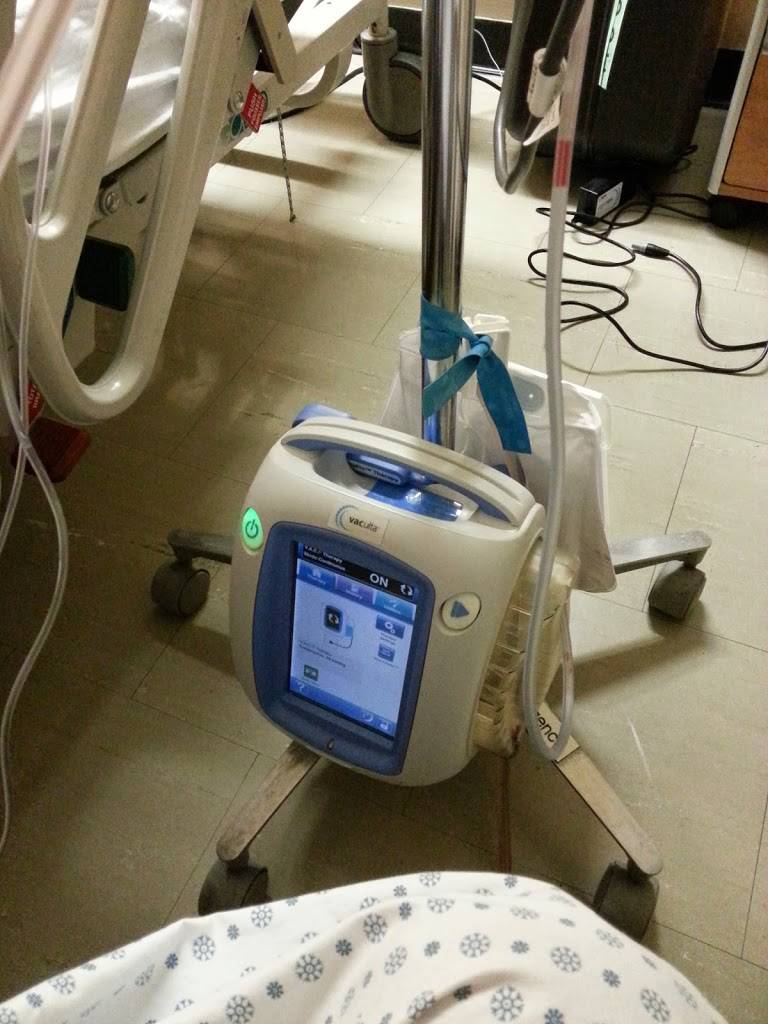
I received my home VAC unit on Nov 16, 2013 and the nurse had come in to set me up that day.
Sitting was impossible at this point due to the pain, so my days were spent laying on my back or standing. The VAC is used to provide negative-pressure wound therapy and is often used as an alternative to packing or suturing a large wound.

The VAC will have either no sound or a very faint hum when it’s working. If the seal is broken, then the unit will become loud and possibly give off an alarm tone.
Unfortunately, my unit was defective, and it was giving me trouble day and night.
Even if there was a perfect seal, I’d get an alarm telling me to check the seal or that there was a blockage. I truly believe that had my unit been working correctly, my recovery would have been significantly shorter.

The VAC dressing was changed every three days. This was extremely painful for me and even with an adhesive remover spray, it was painful to remove the dressing film.
In addition to the film, another part of the problem is that the sponge that’s packed in the wound will stick to the healing tissue and when it’s pulled, it hurts.
The nurse would often saturate that sponge with water or saline in an attempt to loosen it from the new tissue, but that technique could only do so much.
As the wound got smaller, the pain became less severe. Itching was also a problem, and I spent countless nights with the worst possible itch I could imagine underneath the VAC dressing film.
The problem with the film is that you can’t scratch your itch no matter how hard you try – it’s like trying to scratch someone’s nose through a window pane.
This could be due to the fact that as a male, I’ve got hair growing in places that shouldn’t be covered with adhesive film.
The wound was shrinking at a very fast pace during this time, and was less than half its original size only one month out from surgery. I was amazed to see the progress through the photos I’d take with every nurse visit.
Because of the awkwardness of the vac dressing, I began kneeling in front of the toilet to empty my ostomy pouch. It’s been my preferred way of emptying my pouch ever since (Update: Still is eight years later!).
My diet didn’t change after surgery, and I continued to eat whole foods without issues.
Since the ostomy was already there before this procedure, and it wasn’t being disturbed, there really wasn’t anything to worry about.
One thing I’d like to note is that a proctectomy can affect sexual function, especially in men, where there is a risk of erectile dysfunction.
Age seems to be a factor, but the complexity of the surgery required also plays a part.
My surgeon brought this up well before my surgery, and you should talk to your surgeon about this risk if you’re planning to have the surgery in the future.
I had no problems resuming intimacy after the procedure, even with the VAC unit attached to my bottom.
I’ve experienced no pain during sex or during an orgasm at any time following this surgery.
For women, there may be some pain with sex for a few months after the rectum is removed, as it changes the position/shape of the vagina.
That could mean trying different positions in order to get comfortable for the first little while.
From what I’ve read, most women say that those pains go away eventually.
The UOAA has a great guide for intimacy after surgery. The guide can be found HERE.
Stay tuned for PART THREE and FOUR.
I will link the timeline file at the end of part four.





old post i know- but just wanted to leave a tip- buy yourself a gel or memory foam kneeling pad for when you kneel to empty pouch- I didn’t use one for almost 30 years- and my knees looked like camel knees- very calloused and kept getting infections when the callouses would crack open-
I’m facign rectal stump removal due to cancer in the stump (I have Crohn’s- and iliostomy since 1982) Stump developped cancer- so it’s gotta go-surgery is 2 days from now- and I’m panicking- I’m sitting here thinking that in 2 days I won’t be able to sit here for a good long while- especially if complications arise- which i guess they are likely to as from what i understand nearly 50% have complications- ugggh- I’m panicking about going into surgery feeling ok- and waking up in recovery room and realizing I’m in for a long miserable recovery most likely- The pain i don’t care too much about- but the possibility of wound that won’t heal- the leaking- the VAC unti use- the smell- havign to have a nurse help for who knows how long- Blah! I just can’t get over the fact that this is happening- oh well- Anyway- thanks for your posts on Crohn’s and illiostomies and such- been a help-
Hey Bob,
Thanks for the tip regarding those knee pads!
I hope your surgery goes well. My experience was a little worse than what many people I talk to go through, so I’m sure you’ll be fine after the short recovery period!
Wishing you all the best.
Eric
Hi, what a great blog. I had my AP Resection (Proctectomy) on 7th Nov 2015, a little ironic exactly 2 years after yours. I also had peri-anal disease/Crohns Ileo-Colitis. It is so helpful and useful to understand the post op implications and that the pain I am/have experienced is ‘normal’. Very informative and thankyou for having the confidence to share your experience/surgery. Hope you remain symptom free.
Thank you, Tracy! I hope you have a speedy recovery.