Blockages and partial blockages are a concern for ostomates, especially ileostomates, but there are several ways to both prevent and treat minor blockages.
In this article, I’ll go over some tips that I’ve found to be helpful in my own experience, but these tips shouldn’t replace the advice of your care provider.
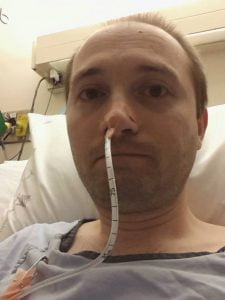
Caution: Blockages are no joke, and I’ve been sent to the hospital because of one. If you feel that you might have anything more than a partial blockage, you should visit your local ER just in case.
Table of Contents
Video
By playing the above video you agree to YouTube's Terms and Conditions and Privacy Policy
Causes of Blockages (Also Called a Bowel Obstruction)
Blockages can be caused by a number of reasons, but not all causes are in our control.
Some ostomates, for example, have strictures or motility issues that increase the chance of blockages. These people should work with their doctor to find solutions that help prevent blockages, including surgery.
Pregnancy, especially in the second and third trimesters, is a risk factor for bowel obstructions as well. If you are pregnant, it’s best to work with both a stoma nurse and an obstetrician to make sure that things go smoothly and you can plan what for what happens if any complications arise.
But for the majority of ostomates, blockages have to do with what and how we are eating.
A small group of ostomates may also experience blockages because their appliance is being put on too tight, and this can be especially problematic in the weeks following surgery when the stoma is more swollen than normal.
Preventing Blockages
If your blockages are being caused by digestive issues, including structures, then it’s important that you’re following up with your GI or surgeon.
The tips below may or may not help if you’ve got problems that are unrelated to your stoma.
What you eat / How you Eat
I’m willing to bet that the majority of blockages are caused by what, or more importantly, HOW we eat. This is actually good news since it means that we’re in control most of the time.
Typically, ileostomates are told to avoid certain foods, especially in the weeks following their surgery. I do have a more complete list of these foods HERE, but for the most part, they include:
- Raw fruits and vegetables.
- Whole nuts and seeds.
- Beans and legumes (especially when dried & cooked).
- Mushrooms.
- Whole corn kernels
- Other, similar foods.
I’ll be honest, I’m not the type of person who avoids foods, especially healthy foods, in order to prevent a blockage. Instead, I make sure that I focus on how I’m eating those foods.
Here are my tips for avoiding food-related blockages:
- Take your time. Eating should be something to do mindfully, and when you rush, you aren’t giving your body the time to chew, digest and assimilate your meals properly.
- Chew!! Perhaps the most important thing you can do is to chew your food until it’s nearly liquid! This is especially important when eating something like mushrooms, which don’t break down in your stomach or gut.
- Go easy on your portion sizes! I tend to eat a few meals throughout the day, but my meals are often huge. This can be problematic, even you’re eating mindfully and pacing yourself. Certain foods are easier to digest than others in large quantities, but if you’re able to eat less food at a time, you’ll be doing yourself a favor.
- Drink with your meals. Drinking before, during and after a meal will help to move things along and prevent your output from becoming too thick and slow.
- Experiment with new foods slowly. This is crucial in the first month or so after your surgery, and you should try small portions of new foods to see how it affects you before using it in a full meal.
- Keep a food diary. You may find that certain foods are more problematic than others, so it might be helpful to keep a food diary until you feel comfortable with the food you regularly eat.
Signs of a blockage
If you’re unfortunate enough to have a blockage, there are symptoms that seem to be common among ostomates.
Keep in mind that these may still vary from person to person, but I’ve experienced the following symptoms myself:
- Decreased or no output over a prolonged period of time.
- Unexpected liquid output that’s out of the norm.
- Pain and/or pressure behind my stoma.
- My stoma will retract.
- Nausea.
- Vomiting (this is a very bad sign!! Get to an ER if your blockage has lead to vomiting!).
I find that certain symptoms, like pain and pressure, can come on suddenly, while nausea and vomiting tend to happen much later (like 12+ hours after the blockage started). Again, this may differ from person to person.
Things I Do When I’m Experiencing a Blockage
When I feel that I’m experiencing a partial blockage, I tend to do the following:
- Drink warm water or tea. This not only helps to flush my digestive system, but I find that warm fluid also help me relax (which is important to do in a situation like this).
- I apply gentle pressure around my stoma and massage my abdomen. I’ve been told that many blockages are just behind the stoma, so massaging the area may help to loosen things up and get things moving again. You may find that some areas around your stoma are tender, so be gentle!
- I’ll bend forwards, backward, sideways, and twist; I may also try to bring my knees to my chest (either while laying down or standing). I find that these movements can also help to push things along.
- I may remove my appliance to give my stoma more space to open up. If your appliance is too tight around your stoma, it could cause the flow of your output to be slowed down. This will help when you’re using the massage technique, but I’d suggest hanging a “kitchen catcher” bag off your pant waist so it will catch any output. You might also find that removing your appliance and massaging while under a warm shower can be quite effective.
Other Suggestions
- Some people like to take a warm bath when they feel a partial blockage coming on. If you do decide to have a bath, keep your appliance on.
- A heating pad may also work as an alternative to having a warm bath.
Things NOT to do
- Do not take laxatives. Taking a laxative if you are partially or completely blocked may cause some serious complications. I would also suggest not drinking liquids (like prune juice) if you have a complete blockage.
- Do not eat until the blockage is resolved. As with laxatives, you don’t want to eat when you’re experiencing a blockage. When was the last time you unclogged a toilet by flushing paper towels down the drain? Same situation here.
- Do not stick anything into your stoma unless a healthcare provider has given you specific instructions. Some ostomates who experience frequent blockages may be given a Foley catheter along with instructions on how to use it on themselves, but this should not be attempted without the OK from your doctor, surgeon or stoma nurse.
- Do not ignore pain or vomiting! If you’ve got enough pain that you’re wincing or have vomited, then you should have been at your doctor’s office or ER a half hour ago! Seriously, don’t ignore these signs.
Tip: It may help to keep a special card to keep on you when visiting your ER. This card is available from the UOAA and can be downloaded and printed HERE
Further Reading
You might enjoy some of my past articles detailing my experiences with partial and full blockages. Please, learn from my mistakes!
Question: Have you experienced a blockage? What helps you?





I’ve also heard that! If I had a colostomy, I’d be all over doing irrigation! LOL
I have an ileostomy and was told this past April I have a partial blockage and my intestines have ballooned to the size of a golf ball. Yet I’m not a candidate for surgery?? I’ve had 17 intestinal surgeries due to Lupus Mesenteric Vasculitis. I am in pain and throwing up. I can’t eat anything or else it gets stuck. I need to go to the ER and skip what the “Specialist” said. Living in a rural area in SC doctors are limited. Yet the specialist I saw is from MUSC number 1 hospital in SC. But doesn’t mean he is a #1 doctor. I’m aggravated to say the least
@Cathy That must be incredibly frustrating and I’m sorry that you’ve had to experience that. Was there any reason given for you not being a candidate for surgery?
Sorry vegan, I shoulld have explained in more detail. the guy was doing more of a colonoscopy prep. he used milk of magnesia. as far as function, a better solution to irrigation. but I wonder if its really healthy for a once a week routine?
I looked into irrigation, not as wonderful as first thought. it takes time and requires more or less a 2 piece bag and other gear-a long drain bag. as I recall about 1/2hr to 45minutes a day or every other day. for me, thats too much time wasted. apparently its not an easy process for I have read about peoples problems in trying to irrrigate. the stoma caps really are not much smaller than a bag. I first assumed they were only maybe 2inches wide. a little bottle cap thing.
i also wonder if constant irrigation is good for the body? hard to think that the lower section of the large intestine only serves as a holding tank. with 10inches of mine gone, I seem to drink a lot more water.
@dogtalkerer I have limited knowledge of colonic irrigation for people who have a colostomy (since I don’t have one myself), but I’ve heard from stoma nurses who say that once patients get over the initial learning curve, it can help to make things far more predictable and easier to manage.
Some benefits include the ability to wear a “stoma cap" instead of a large bag between irrigation sessions. It can also, depending on the natural stool transit time of the person, help to delay output by days – a huge benefit for some.
Yes, it does take some time and extra equipment, but this could be worth it for many. Of course, if someone has a “slow" colostomy that needs to be emptied every few days, then it may not offer many benefits.
I’m not aware of any harm for a colostomate to do this, although I would love to see studies on how it could impact our gut flora. Your observation about needing to drink more water doesn’t surprise me.
@veganostomy While I don’t irrigate regularly, it is a godsend when I do. Yes, it takes time – for me, it takes a couple of hours just to be sure I don’t have any “late returns “ but I think if I did it more regularly, it would take less time as I became more efficient. I only irrigate when I need a stretch of time free from interruption. So if I am going to dinner and theatre, I don’t want to be constantly heading to the loo. When I irrigate, I can generally count on 36 hours free from output, sometimes more. I know that lots of colostomates irrigate daily, but it isn’t a need for me.
It isn’t a difficult process at all, however, it takes some practice. I would be happy to walk anyone through the process if they’re thinking of trying it. I even got Coloplast to send me the irrigation kit for free.
@tigerlily
Wow wee! I would love to be regular again, but am a little nervous about trying anything new. I never know when I am going to have output. Some days it’s in the afternoon, others in the evening, and other times first thing in the morning, but mostly on and off all day.
Stella
@sjlovestosing Yeah, I am pretty much the same. What I hear from people who irrigate regularly is that it trains your body to a schedule. I don’t irrigate enough to know if that is the case, but it’s nice to have some freedom when I do. If you’re interested in it, have a look at YouTube videos on the subject. They are really helpful. It seems daunting the first time, but it isn’t as complicated as you think. You might find that you like it.
Laurie
@tigerlily
Thank you, Laurie, I will do that!
Stella