It seems rather silly that I even have to make a post about this, but unfortunately the information on the Hollister website isn’t very clear (no pun intended).
Tips
My first ileoscopy
It’s all done. Over with. Finished. I was given my first ileoscopy yesterday and it was an interesting experience to say the least!
Ileoscopy prep – getting scoped through a stoma
On July 9th, 2014, I was scoped as a follow-up to my ostomy surgery and to also make sure that my Crohn’s hasn’t spread to my small intestine.
Hollister Ostomy Pouch Hack – OSTOMY TIP (w/ video)
I’ve been trying a new Hollister ostomy system out, and I immediately noticed something that I found rather annoying: the pouch outlet just dangles from the bottom.
Those damn blockages…
Yesterday, I had a pretty normal morning… emptied my pouch at 7am and then again at 10:30am. For brunch, I had some leftover rice with avocado, followed by two medium-sized apples.
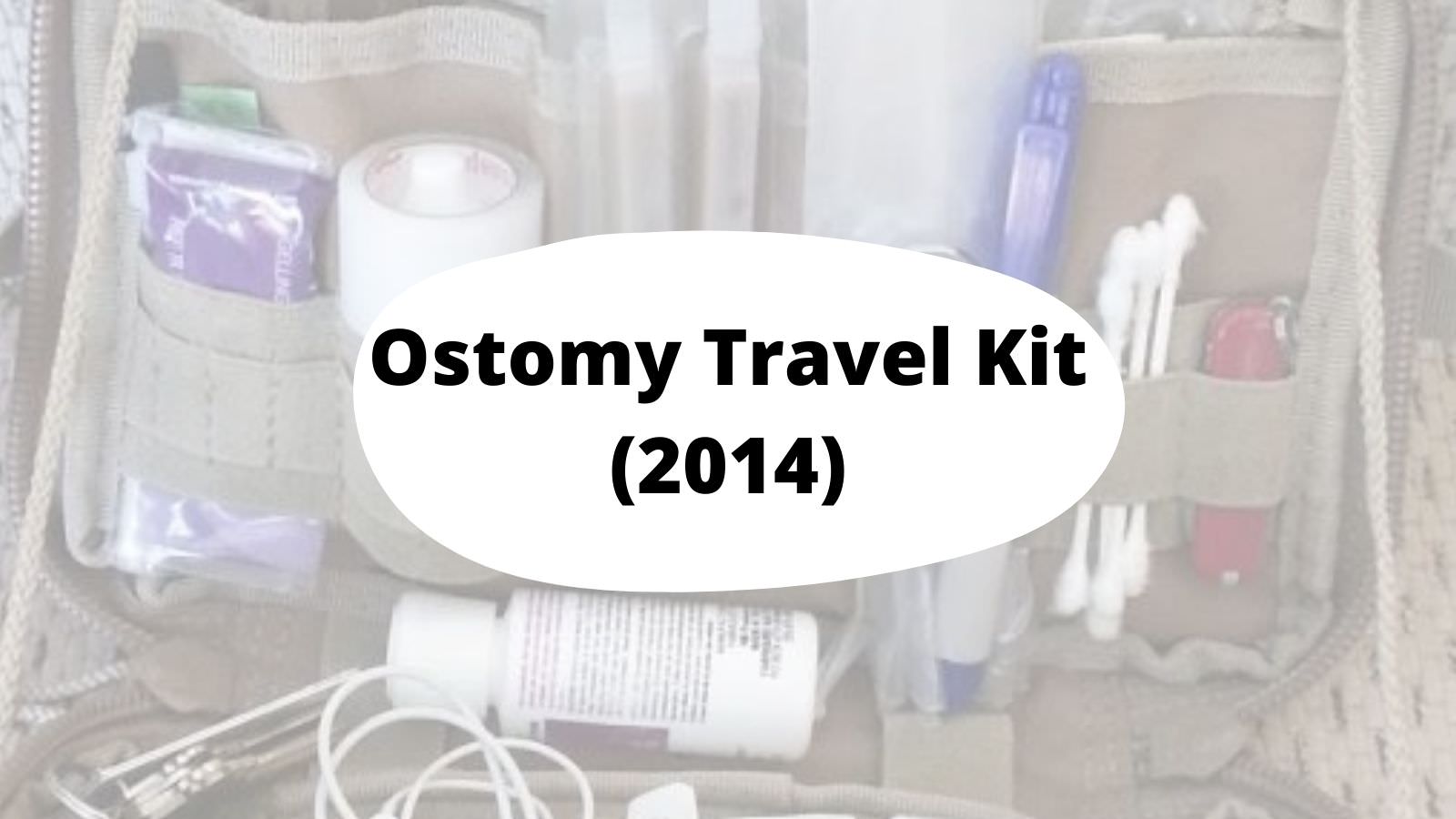
My Ostomy travel kit – Feb, 2014
Inspired by another fellow blogger, I’ve decided to finally get a proper EDC (every day carry) bag for my ostomy supplies. This new bag is replacing a MUCH LARGER tactical shoulder bag, which I may still use for hikes or whenever more supplies are needed.
First major leak – meltdown averted
6am on a Monday morning. I wake up in a haze, ballooned pouch at my side, but something was wrong…
Enhancing Nutrient Absorption – TIPS
“IT’S NOT WHAT YOU EAT, IT’S WHAT YOU ABSORB”
When it comes to nutrition, that’s the golden rule. You hear a lot about how eating a healthy diet will improve your health, but that’s only IF you absorb the nutrients from your food. For most healthy people, this isn’t a big problem, but if you have a digestive disorder or if you’re eating a plant-based diet, there are things you can do to enhance the absorption of nutrients.
IBD/Ostomy nutrition – tips
Food substitutions may be required if your digestive problems extend to more than just having a stoma.
Preparing for surgery – what to bring.
I’ll be heading in for my second surgery soon. This time it will be to remove my rectum.